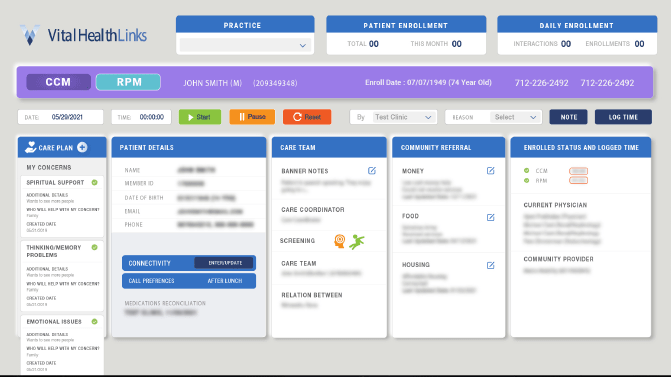
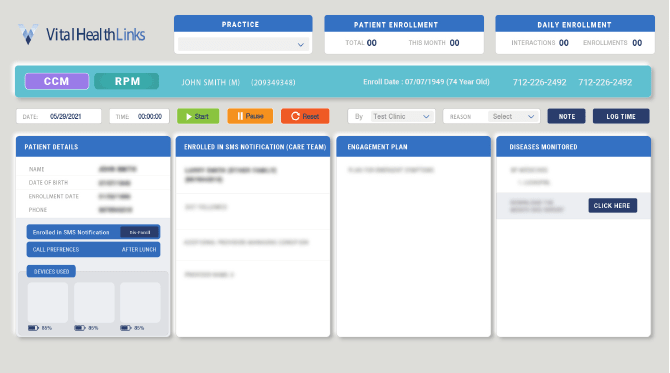
Doctor-led CCM & RPM Maximizes Your
Patient Engagement
Teams & Workflows
Revenue Growth
Patient Engagement
Teams & Workflows
Revenue Growth

Vital Health Links' enhances your practice growth and clinical care through sustainable, full-service Chronic Care Management (CCM) and Remote Patient Monitoring (RPM) supported by doctors.







 Increased Revenue
Increased Revenue
 Reduce Burnout
Reduce Burnout